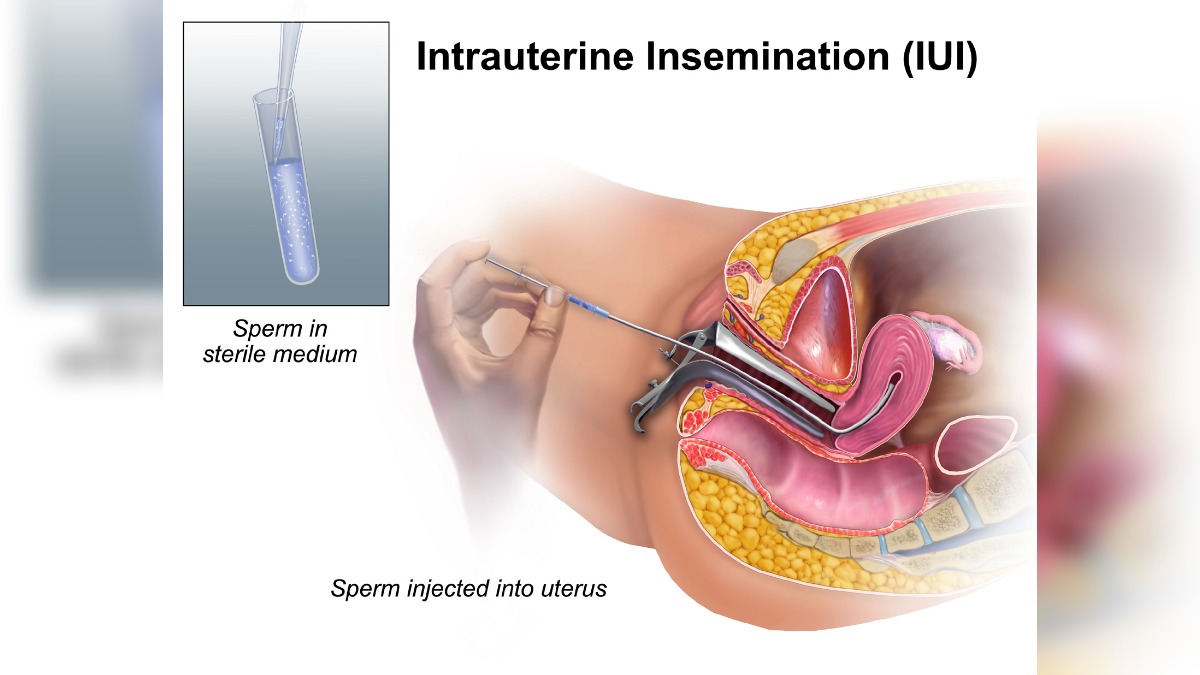
Intrauterine insemination, Artificial Insemination, or IUI is principally the first Assisted Reproduction Techniques (ART) used. IUI, one of the oldest methods of fertility treatment, dates back to the 18th century where the sperm from the male partner is inseminated into the female reproductive tract for fertilization and pregnancy to take place naturally.
IUI, initially known to address male fertility factors, has more diverse benefits with the advancing reproductive techniques and flexibility to be coupled with fertility medications and other ART procedures such as Ovulation Induction.
Through this article, we shall understand the process of IUI, its requirements, cost, success rates, and factors influencing IUI success rates.
Also Read: Intracytoplasmic Sperm Injection (ICSI): What is It, Who Should Opt, Success Rates, Cost, and More
In this Article
What exactly is IUI?
Intrauterine insemination is a process of artificial insemination. Here, the sperm is recovered from the male partner to be placed carefully with the help of a catheter into the uterus of the female reproductive tract through the vaginal opening at the right time of ovulation. The sperm travels through the fallopian tube to fertilize with the awaiting egg. Further, the embryo formed after fertilization moves to the uterus for implantation and pregnancy commencement.
Who are the ideal candidates for IUI?
IUI is for couples who cannot get pregnant despite timed intercourse or fertility medication intervention. Some of the other infertility factors taken care of by IUI are:
- Endometriosis: In women affected with endometriosis-related infertility, medications primarily help retrieve good-quality eggs, followed by IUI, the first line of treatment approach considered.
- Male fertility factors: Men having the following fertility factors can opt for IUI pregnancy as the procedure allows insemination of good quality sperm.
- Low sperm count (oligospermia),
- Abnormal sperm morphology (teratozoospermia)
- Unusual sperm movements (asthenozoospermia)
- Obstructive ducts causing nil sperm ejaculation (Obstructive azoospermia)
- Sperm ejaculated through urine (retrograde ejaculation)
- Cervical factors: The cervical discharge at the time of ovulation ideally favors the sperm to travel through the vagina to the fallopian tubes for fertilization. But, when the cervical mucus gets thick, or the cervix due to scarring thickens. This impedes the sperm journey causing fertilization problems. The IUI process enables the placement of the sperm directly into the uterine cavity, bypassing the cervix.
- Ovulatory factors: For women having ovulation problems such as irregular ovulation, absence, or delayed ovulation, IUI may be combined with fertility medications to regularize ovulation, and the sperm inseminated at the right time of ovulation increases pregnancy chances.
- Donor sperm considerations: Women considering donor sperm to get pregnant can use IUI. Here, cryopreserved sperms are thawed before IUI.
- Human seminal plasma hypersensitivity (HSP): Very rarely, seen in women, is an allergic reaction to the protein in men’s semen. In such women, the contact of semen on the skin or vagina causes irritation, redness, swelling, and persistent burning. IUI can be effective in such cases where sperm processing removes many allergy-causing proteins in the semen.
- Unexplained infertility: When the reason for infertility is not known, IUI is the first line of treatment performed along with ovulation-induction (OI).
What are the Prerequisites of IUI?
Artificial insemination requires preparations before its actual procedure. They include:
- Preparing the semen sample: The semen sample collected through ejaculation or surgical aspiration techniques needs washing, and highly active or normal sperms must be separated. In the case of frozen sperm or donor sperm usage, the sperms require thawing before IUI.
- Determining the right time of ovulation: The timing of IUI is the key, and so, monitoring for signs of approaching ovulation is crucial. Blood assays and Ultrasound imaging can confirm the same. Women undertaking hormonal medications for ovulation may require a trigger shot of hCG or human chorionic gonadotropin for the ovaries to release more than one egg at the right time of ovulation and improve the chances of pregnancy.
- Patent fallopian tubes: At least one functional fallopian tubule is required to have a positive IUI outcome.
IUI: The treatment process
The treatment process of Intrauterine insemination involves the following steps:
OVULATION INDUCTION
(For women with ovulatory disorders, ovulation-inducing medications are given from day 2 or 3 of menstruation for 8-12 days with constant ultrasound monitoring)
↓
hCG ADMINISTRATION
(36 hours before insemination of sperm, hCG, the trigger shot given to stimulate the ovaries releases one or more eggs)
↓
SEMEN SAMPLE COLLECTION and PROCESSING
(On the previous day or same day of IUI, semen samples are collected. The frozen semen sample thawed before use, is processed in the lab, and good quality sperms are segregated)
↓
INSEMINATION OF SPERMS
(The sperms are placed with the help of a catheter inserted through the vagina into the uterus. The sperm swims to fuse the egg waiting in the fallopian tube.)
↓
MEDICATIONS AND Serum Beta hCG TEST
(Medications for 14 days to support the uterine growth and thickening for an upcoming pregnancy. Nearly 14 days post-IUI, pregnancy tests are done to confirm IUI pregnancy)
What are the Success Rates of IUI?
Intrauterine insemination has helped many conceive and is an effective procedure for eliminating various infertility factors. Women undergoing IUI may find vaginal spotting, slight discomfort after the sperm placement process. IUI promotes the release of more than one egg. And so, the possibility of multiple conceptions with IUI is more. It is inevitable to say, every couple’s IUI outcome is different, and the success of IUI is dependant on a range of factors such as,
- Age; success rates are low in older women (above 40 years)
- Underlying fertility issue
- The procedure and medications used.
However, The IUI success rate in women above 35 years is almost 20%, the IUI success rate in women above 35 is 10%, and above 40 is only 2-5%. It is also important to note that at least three Insemination cycles are proven beneficial. And doctors may recommend an IVF only after three failed insemination cycles.
How much does IUI cost?
IUI is a highly affordable fertility treatment procedure. The cost of a single IUI cycle is almost INR 3,000 to INR 5,000. The base cost excludes fertility medications, lab tests, and ultrasound scans. The overall cost of one IUI cycle (everything included) may start from INR 10,000. This cost varies between individuals, clinics, and cities.
Frequently asked Questions
Conclusion/ Take-Away
IUI or insemination of sperm into the uterus of a female is a simple procedure addressing major male fertility factors and certain female infertility conditions. Though 80% of pregnancies with a minimum of three IUI cycles is possible, couples having an IUI failure may consider IVF to counter their fertility issues. You will need to further connect with a fertility specialist to understand your chances of pregnancy through the IUI cycle or undergo a fertility treatment for your infertility condition.
References:
Overview| https://academic.oup.com/humupd/article/15/3/265/750532