Pregnancy is a beautiful journey allowing expecting mothers to experience even a small change in their body – the heartbeat of the baby, the baby’s growth and movements, fundal height changes, the weight gain, and the list goes on. Among the various profiles tested during pregnancy, adequate liquor levels- a foetal biophysical profile is indispensable.
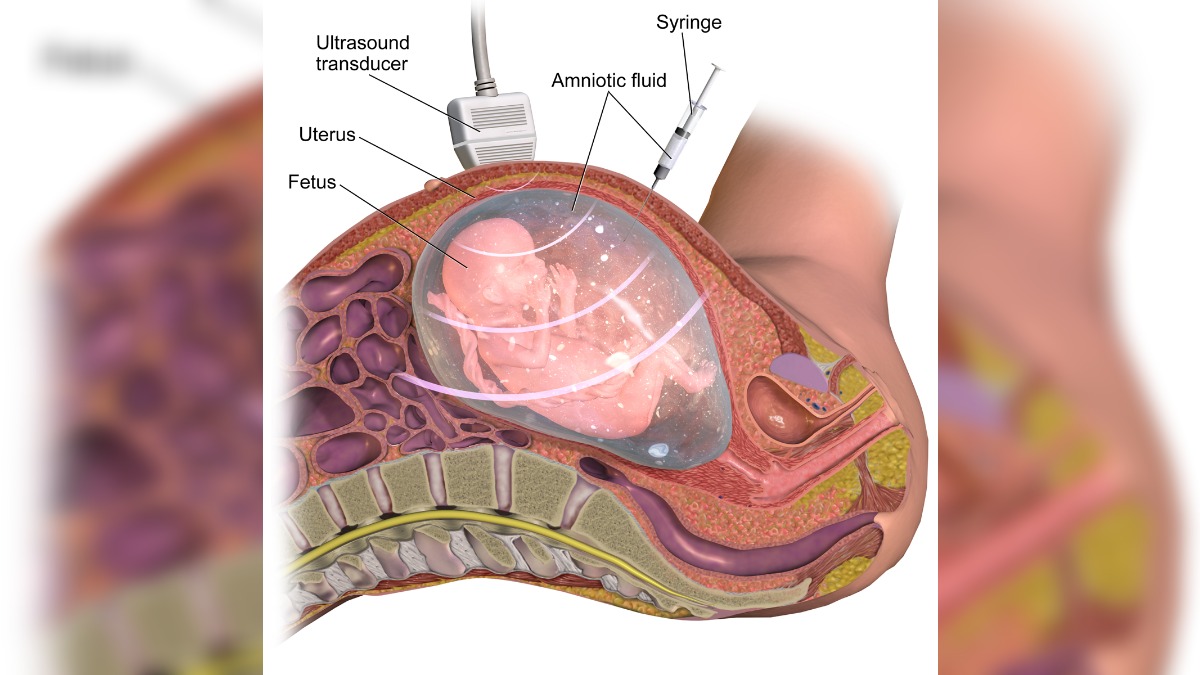
When we talk about adequate liquor levels in pregnancy, the term liquor refers to the amniotic fluid surrounding the baby during its growth in the womb. Adequate liquor level in pregnancy, known as Amniotic Fluid Index or AFI, is a vital parameter of foetal development that needs to be within normal levels, otherwise can impose risks to both the mother and the baby.
Through this article, you will further explore what Amniotic Fluid is all about, the normal range of AFI required for a healthy pregnancy, and ways you can treat low or high amniotic fluid levels.
Also Read: BPD And FL Chart in Pregnancy – Biparietal Diameter and Femur Length in Ultrasound
Get a consultation with the best specialist in your Location
In this Article
Amniotic fluid and its composition
Did you know that your child swallows the amniotic fluid, and it helps the baby float inside the womb? Amniotic fluid, present in the amniotic sac, is a clear, pale yellow liquid. It is a workstation that:
- Cushions the developing baby,
- Allows proper bone growth and organ development,
- Allows the baby to move,
- It helps prevent exertion on the umbilical cord,
- It helps maintain a constant temperature around the baby and regulates the baby’s temperature.
The body starts producing amniotic fluids as early as 12 days after conception. This vital fluid comprises water and electrolytes drawn from the mother’s plasma until week 12 of pregnancy.
During the second trimester, proteins, carbohydrates, lipids, and urea are added to the amniotic fluid aiding in the baby’s growth.
From week 16 of pregnancy, when the foetal kidneys begin to function, the urine generated becomes the prime source of amniotic fluid.
Also Read: TT Injection in Pregnancy: Why is It Given, in Which Month, Side Effects, and More
It may seem strange, but the cushioning effect and the baby’s means of survival in the womb is the liquid waste it leaves behind. As said before, amniotic fluid is an essential component for the baby’s growth, composed of:
- Nutrients – zinc, copper, folate, and iron.
- Hormones – prolactin, prostaglandins, steroid hormones, proteins, progesterone, androgens.
- Skin protectors of the baby – Vernix and lanugo shed into the amniotic fluid
- Antibodies – transmitted from the mother, placenta.
What is the Amniotic Fluid Index (AFI)? How is it calculated?
Amniotic Fluid Index or AFI is the score given to the level or depth of amniotic fluid when viewed on ultrasonography. AFI increases with advancing pregnancy and baby growth until the baby reaches 32 weeks of gestation. After which, the level remains constant until the completion of the 37 to 42 weeks of the pregnancy term.
During the first two trimesters, ultrasound scans of the uterus measure the deepest pocket of amniotic fluid called “ maximum vertical pocket (MPV)” or “single deepest pocket (SDP).” The optimal MPV or SDP levels range between 2 -8 cm, where 2 cm indicates a low amniotic fluid stage.
Also Read: Ovary Normal Size in mm: Right and Left, Is Ovary Size Important to Get Pregnant?
During the third trimester, AFI is the most common parameter used that measures similar to MPV or SDP ultrasound procedure. The only difference is the ultrasound technician will measure fluid pockets at four different sections of the uterus to determine the AFI measurements (the sum of all the four values obtained).
| Amniotic Fluid Index (AFI) = Sum of 4 values obtained from 4 different pockets of the uterus |
| The Normal Amniotic Fluid Index (AFI) range is 5 to 25 cm. |
What does abnormal AFI indicate?
There are two possibilities of abnormal AFI conditions mentioned in the table below.
| Abnormal AFI Condition | Pregnancy complications | Indications | Treatments |
| 1. Excess amniotic fluid levels around the baby or polyhydramnios – AFI Measuring above 24 cm- occurring only in 1% of the overall pregnancies having chromosomal anomalies, multiple pregnancies, and gestational diabetes. | It is not a sign of any significant complication. Still, it can cause pregnancy risks such as:
Preterm delivery Prolapsed umbilical cord (dropping out of the cord through the cervix by breaking the vagina) Early water bag collapse Excessive bleeding after childbirth Baby with a health condition. |
Gradually developing condition having noticeable symptoms like:
Breathlessness Swollen feet and ankles (edema) Heartburn and constipation. However, these signs may not necessarily be caused due to polyhydramnios. Ultrasound scans can confirm this condition. |
Extra prenatal scans and ultrasound to check the health status of you and the baby
Changes in diet, medications (diabetes medications) Medications to stop more fluid production or draining of the fluid using a needle. |
| Low amniotic fluid levels or oligohydramnios – AFI measuring below 5 cm and MPV or SDP less than 2 cm-
caused due to high blood pressure, preexisting diabetes, placental issues, obesity and dehydration in mothers |
Oligohydramnios in first two trimesters can pose higher complications than 3rd trimester such as:
Birth defects, Preterm birth, miscarriage, or stillbirth Pregnancy complications during trimester three are: Slowing down of baby’s growth Labour complications including umbilical cord compressions restricting baby’s food and oxygen supply
A greater possibility of a caesarean delivery |
Noticeable signs of oligohydramnios include
Premature rupture of membranes (PROM) before labour Low maternal weight Leaking of amniotic fluid from the sac Abdominal discomfort Sudden drop in foetal heart rate and reduced foetal movements |
Increase your fluid intake
Amnioinfusion – Squirting of saline water through the cervix into the amniotic sac Amniocentesis to inject fluid into the amniotic sac IV fluids for dehydration treatment Changes in diet and medications Ample bed rest with restricted physical activities Extra monitoring to check the baby’s heart rate, movements until delivery or week 36 of pregnancy. |
Get a consultation from the best IVF center of your Location
Conclusion
Adequate liquor levels during pregnancy or optimal Amniotic Fluid Index is a foetal biophysical profile component assessed during an ultrasound scan. The normal AFI range is between 5 cm and 25 cm. Conditions above or below normal AFI can cause complications in pregnancy and labour difficulties. Regular prenatal check-ups, ultrasound scanning, and necessary treatment or precautions can avert potential pregnancy risks consequent of abnormal AFI.
Reference
- Overview | Medline plus
- Science direct